Lung Biopsy
A medical procedure where a tissue sample is
taken from the lungs to be examined under a
microscope for signs of disease, including cancer.
The aim for lung biopsy is to obtain tissue sample from the abnormality shown on your scan for pathology examination. It is often performed to rule out or confirm cancer, or other diagnosis such as infection or inflammation.
By the time you book your lung biopsy with us you should have had a discussion with your own doctor and a good understanding as to why you need a lung biopsy.
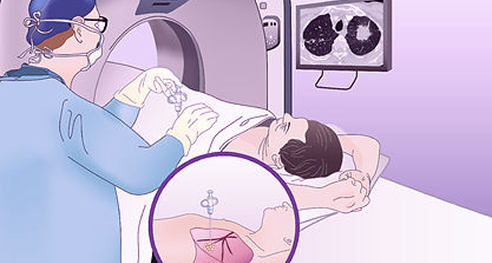
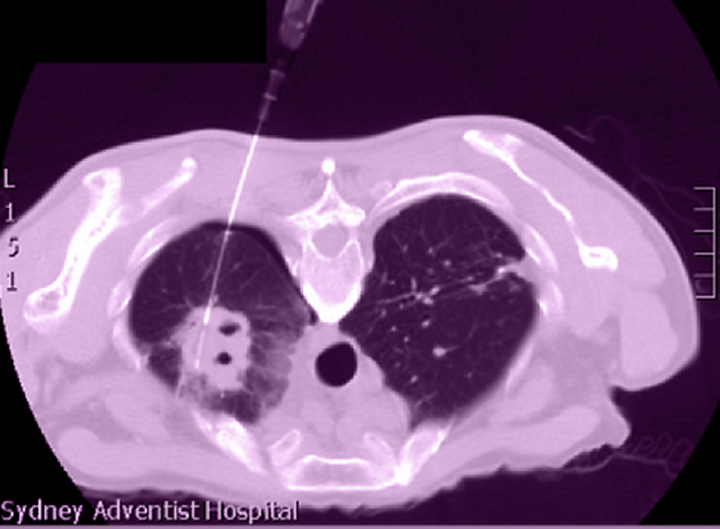
We now perform all lung biopsies under CT guidance which is precise and therefore ensures accuracy and safety. You will be lying on your back or chest depending on whether the biopsy is from the front or the back. You will be given intravenous sedation as well as local anaesthetic.
What is the difference between fine needle aspiration biopsy (FNAB) and core biopsy?
FNAB was the traditional way of performing lung biopsies. A fine (skinny) needle is inserted into the abnormality to aspirate (suck out) cells and materials. Quite often material obtained by FNAB is insufficient for definitive diagnosis. We now perform all our lung biopsies using a core biopsy needle so that small tissue pieces are obtained. We have conducted our own studies at the SAN, showing that core needle biopsy provides a better sample, is quicker to perform and is as safe as FNAB.
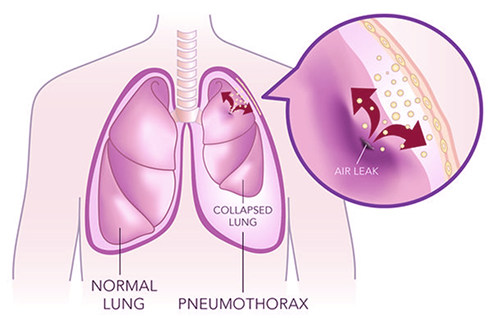
The main risk is pneumothorax (collapse of lung). We use CT to check for pneumothorax immediately after lung biopsy. Tiny and small pneumothoraxes are quite often detected (30%). Large pneumothorax is rare (<3%) and requires insertion of a mini drain from the front of the chest. You might cough up blood, but this is self-limiting. Mild pain and bruising may be present at the needle entry site. Significant bleeding complications are very rare (<1%).
We will keep you under observation for about 1-2 hours. You will need to arrange someone to drive you home since you cannot drive for 24 hours after sedation. You should also have someone staying with you overnight in case you developed shortness of breath.
If you had a pneumothorax, a chest X-ray will be taken to make sure it is not getting worse before we send you home.
We would prefer anticoagulants (such as Warfarin, Heparin, Clexane, PradaxaXarelto, and Eliquis) and antiplatelet (such as Plavix) drugs to be stopped for some time before the procedure. However, we do not know the exact reasons as to why you need these blood thinners, so we cannot give you the instruction to stop. You will need to check with your GP or specialist, who started you on the blood thinner, whether it would be safe for you to stop (Warfarin for 4 days, Plavix for 4 days, Clexane the night before). Aspirin is preferably stopped for 4 days as well if possible. If the blood thinners cannot be stopped, then you need to discuss this with your referring doctor regarding the value of the biopsy against potential bleeding risk.
Development of worsening chest pain and shortness of breath indicate enlarging pneumothorax and you need to be taken to a hospital emergency department immediately. If the symptoms are severe, an ambulance should be called.
The pathology result will be sent to the referring doctor. You will need to make an appointment to see the referring doctor to check your result, which should be available in a few days.
Our interventional radiologists need to see your scans to plan for the biopsy. If you had your scans done with SAN Radiology, PRP Imaging or I-med Imaging, we can view your scans online. If you had your scans done elsewhere, please bring in the films or CDs for review and planning. Ask your referring doctor to fax through your referral letter with your contact phone number. Once our interventional radiologists have finished planning, we will ring you regarding the appointment.
Drive to the Sydney Adventist Hospital on 185 Fox Valley Road Wahroonga.Park in Carpark P1. Take lift to Level 4. Proceed to Day Admission Centre at Level 4 Tullock Building for Admission, and then come down to Level 3 San Radiology CT Scanning Section to have your procedure.