Portacath
A medical procedure where a tissue sample is taken from the lungs to be examined under a microscope for signs of disease, including cancer.
A portacath is an implanted venous access device for patients who need frequent or continuous administration of chemotherapy. Drugs used for chemotherapy are often toxic, and can damage skin, muscle tissue, and sometimes veins. They often need to be delivered into large central vein where the drugs are immediately diluted by blood stream and delivered efficiently to the entire body. Cancer patients also require frequent blood tests and scans to monitor their treatments. For patients with difficult veins, it can be used for withdrawing blood for blood tests, as well as diagnostic scans.
Using modern techniques, the portacaths we have inserted are highly appreciated by patients, oncology nurses and doctors. The procedure is easily performed with minimal risk and pain.
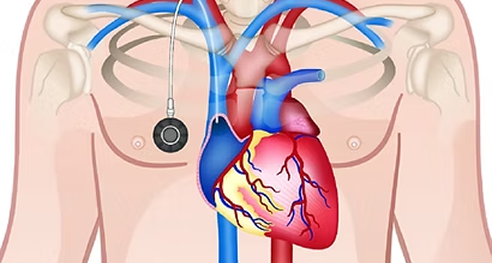

A portacath consists of a reservoir (the port) and a tube (the catheter). The port is implanted under the skin in the upper chest. It may appear as a bump under the skin in thin patients, but less visible in patients with some subcutaneous fat. The catheter runs in a tunnel under the skin, going over the collarbone and then enters the large vein in the lower neck (the internal jugular vein). Since it is completely internal, swimming and bathing is not a problem. The septum of the port is made of a special self-sealing silicone rubber. It can be punctured up to one thousand times and therefore can be used for many years.
The procedure is performed under local anaesthetic, with the aid of imaging guidance (ultrasound and X-ray) in the angiography suite of radiology department. The actual procedure takes about 30min. An intravenous sedation is given to make the local anaesthetic injection less painful. There will be a skin incision 3cm long on the chest wall for the port pocket and a 5mm nick in the lower neck to enter the vein. Absorbable sutures are used for the chest wound and are buried under the skin. For the small neck wound, sutures are usually not required and the wound is closed with Steristrips (medical sticky tape).
Typically you can go home two hours following the procedure, when you have recovered from the sedation. You should arrange someone to take you home, as you are not allowed to drive or operate machinery for 24 hours.
You need to avoid solid food from midnight. Usual medications with a small amount of water is allowed up to the time of procedure. If you are on aspirin, Warfarin or Plavix, check with your own doctor to see if these can be stopped for 4 days. You can resume these medications the day after insertion. Insertion is best delayed if you have active infection.
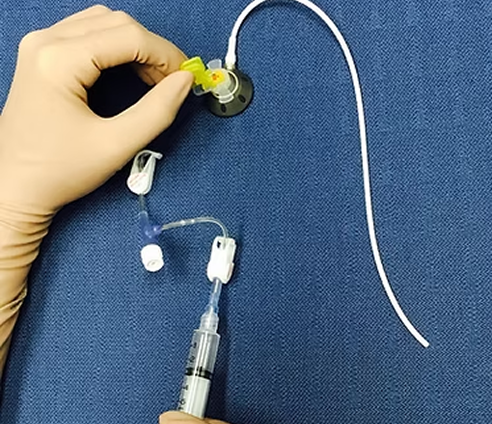
For 5 days you need to keep the wound clean and dry, and to avoid strenuous activities of the upper limb and chest wall. If you will commence chemotherapy within the next two days, please let us know so that we will leave a Huber needle catheter on the port ready for immediate access; the oncology nurse will apply new dressing when you finish the chemotherapy session.
Any issues associated with the wound healing, please contact us.
When the portacaths are no longer used, it needs to be flushed with saline and locked with heparinised saline once per month to keep it patent.
If the portacath is no longer required, it can be removed by us. The procedure is performed under sedation and local anaesthetic, similar to insertion.
The vein is large and superficial, easily visualized with ultrasound. It runs a straight course towards the right atrium. This vein has the lowest risk of complication associated with insertion and subsequent usage. The left internal jugular vein is the second best.
Application of modern imaging technique has made portacath insertion much safer and quicker. The patency of the vein is checked with ultrasound. The best site for puncture and the course of the tunnel are selected using ultrasound, avoiding other veins and arteries in the area. The actual puncture is performed under real-time ultrasound guidance, thus avoiding injury to the adjacent artery. Once the vein is punctured, a guide wire is inserted and its position is checked under fluoroscopy (X-ray). The length of catheter required is measured with fluoroscopy. Finally the function of the portacath is checked by injection of X-ray dye.
With modern imaging guidance, the risk of the procedure itself is minimal. There are theoretical risks of blood vessel injury, wound infection, bruising and haematoma formation, and the very remote chance of allergic reaction to the X-ray dye and drugs used during the procedure.
Tissue might gather around the tip of the catheter forming a fibrin sheath. This can be resolved by saline flush or clot dissolving agent (Urokinase). Skin irritation from leaked drugs may occur if the Huber needle is not completely inserted into the port. When there is pain in the neck or chest, chills and fever, you need to report to the treatment team immediately as the port might be infected. Urgent antibiotic and port removal might be required. Pain and swelling in the neck may indicate underlying thrombosis. You need to report this immediately to your treatment team.
IR is a subspecialty of radiology. Interventional radiologists apply minimally invasive therapy using imaging guidance such as X-ray, ultrasound and CT scan. IR procedures are typically performed under local anaesthetics. Intravenous sedation and analgesia may be required in some procedures. It is generally less risky than open surgery and the recovery is usually faster.